An uncommon but important cause of neonatal bowel obstruction.
Definition
Hirschsprung’s disease (HSCR) is an aganglionisis of the distal gut due to failure of migration of neural crest cells to myenteric and submucosal bowel pexus
Presentation
HSCR can present differently depending on age and severity.
Antenatal suspicion
Neonatal period
- constipation progressing to obstipation
- abdominal distension
- bilious vomiting
- delayed passage of meconium
Hirschsprung’s associated enterocolotis (HAEC)
- constipation with spurious/ overflow diarrhoea
- abdominal distension, with visible , palpable bowel loops
- failure to thrive
- pyrexia
Age at diagnosis varies, and is likely dependent on robustness of health systems and neonatal screening programmes.
- In US, >70% neonatal diagnosis
- In NW Tanzania: ~5% neonatal presentation
Age and Incidence
Rare, 1 in 3500 live births .
Antenatal
Neonatal
Childhood
Adulthood
Sex
Male > Female
Genetics
Most cases of HD are sporadic (80%)
Where there is a pattern of inheritance (20%), the association can be syndromic or familial
Syndromic HD
- Trisomy 21 :
- 3 percent of T21 patients have HSCR.
- 7% of HSCR patients have T21.
- Neurocristopathies (disorders of neural crest cell differentiation and migration)
- Shah Waardenburg syndrome type IV
- Mowat-Wilson syndrome: Microcephal, characteristic facies, GDD. 50% of MWS patients will have HD. Associated with ZEB2 gene mutations.
- Congenital central hypoventilation syndrome (Ondine’s curse) : autonomic dysfunction syndrome predisposing to sleep apnoea, HSCR (~15%, Haddad syndrome) and neural crest tumours (5-10%). Associated with PHOX2B gene mutations.
- Heriditary neuuroblastoma with Hirschsprung’s disease syndrome (PHOX2B mutation)
- Multiple endocrine neoplasia : MEN2B (RET, GFRA genes). Ganglioneuromas are included in the spectrum of intestinal neuronal dysplasia (IND) . Association with medullary thyroid carcinoma ( RET-620 (the “Janus gene”).
- Heriditary neuuroblastoma with Hirschsprung’s disease (PHOX2B related)
- EDNRB and RET gene mutations implicated
- Progressive penetrance with implications for aganglionic length i.e. increased risk of long segment, total colonic and total intestinal presentations
- Autosomal pattern of inheritance, but penetrance is variable
- Parental transmission ~20%, Sibling risk ~ 10%
Aetiology
Differentials
For neonates presenting with infrequent of delayed passage of stools, consider
- anorectal malformation
- small left sided colon syndrome
- meconium plug syndrome
- meconium ileus
Variants of HSCR: These are conditions with a similar presentation to HSCR, but with ganglion cells identified on rectal biopsy.
Variants described include:
- megacystis microcolon intestinal hypoperistalsis syndrome
- intestinal neuronal dysplasia
- intestinal ganglioneuromatosis
- isolated hypoganglionosis
- immature ganglia
- absence of the argyrophil plexus
- internal anal sphincter achalasia
Diagnosis should be based on histo-immunochemistry and electron microscopy.
Severity/ Staging
HSCR is staged in a segmental approach.
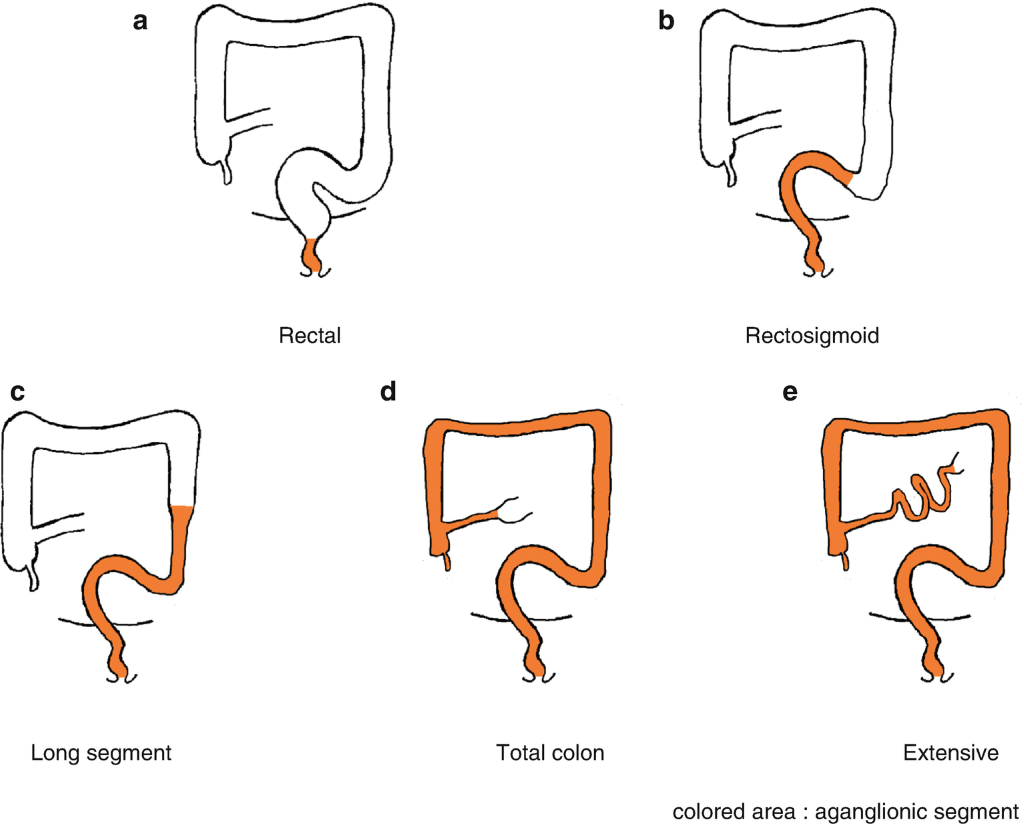
Ultrashort: within 3cm of anus i.e. distal rectum. Characterised by late presentation in childhood.
Short segment/ Rectosigmoid: This is the most common i.e. 75%
Long segment: Involving colon proximal to the sigmoid. ~20%
Total colonic aganglionosis (TCA): ~4%
Total Intestinal ganglionosis (TIA). ~1%. This cohort is unusual due to:
- early presentation with delayed passage of meconium (d4-8)
- collapsed bowel, little or no intestinal distension, no transition zone
- hypertrophic nerve fibres may be absent
- seen more commonly in familial HSCR
Investigations
Bedside
- Abdominal examination
- Digital rectal examination / anal calibration
Blood tests
- CF testing for delayed passage of meconium
- Neonatal thyroid function screen
Specimen
- Rectal biopsy :
- In neonates and younger infants , this can be achieved by the bedside using blind rectal suction. Biopsy forceps include rbi2, Noblett, solo-RBT, Scheye.
- In older infants and children, a general anaesthetic is indicated under direct or endoscopic vision. Strip or cup biopsies are taken.
- Histopathology
- Dual approach of histopathology (H&E) and immunohistochemistry (Calretinin)
- H&E is 85% specific and 100% sensitive
- Calretinin is 97% specific and 100% sensitive
Imaging:
Contrast enema can be contributory towards an HSCR diagnosis.
Special tests:
- RAIR:
- Recto-anal inhibitory reflex is tested on anorectal manometry
- With a false negative rate of 4%, it is contributory toward ruling our HSCR. However, the gold-standard diagnostic i.e. Calretinin immunohistochemistry has 100% sensitivity and 97% specificity. Considering the consequence of a missed HSCR diagnosis, RAIR may be considered contributory but non-diagnostic.
Controversies
Primary versus staged approach
- Primary approach required earlier pull through to avoid HAEC and relieve family from daily washouts
- Pre-operative HAEC ~ increased risk of post operative adhesive obstruction
Age at biopsy